Management Of Temporomandibular Joint Ankylosis
Temporomandibular joint (TMJ) ankylosis is a pathologic condition where the mandible is fused to the fossa by bony or fibrotic tissues. This interferes with mastication,

Temporomandibular joint (TMJ) ankylosis is a pathologic condition where the mandible is fused to the fossa by bony or fibrotic tissues. This interferes with mastication,
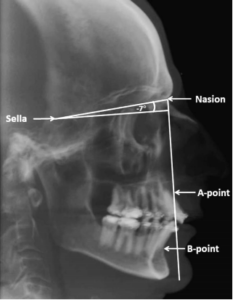
To analyze and compare pharyngeal airflow characteristics pre- & post–mandibular setback surgery in patients with Class III skeletal dysplasia using cone beam computed tomography (CBCT)

This retrospective study evaluated outcomes with the use of calvarialbone grafts (CBGs) in maxillofacial reconstruction as well as donor andrecipient site complications
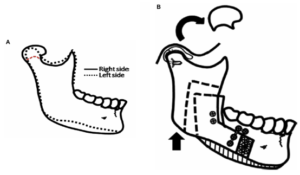
A classification system was developed to place patients with condylar hyperplasia (CH) into categories based on histology, clinical and imaging characteristics, effects on the jaws
This retrospective study assessed the outcome of 603 patients undergoing partial inferior turbinectomies (PIT) in association with Lefort I osteotomy.
Lymphoma is a common disease of the head and neck. Mucosal-associated lymphoid tissue (MALT) lymphoma constitutes a rare type of extranodal lymphoma. The Waldeyer’s ring
In this study, we investigated volumetric and dimensional changes to the pharyngeal airway space after isolated mandibular setback surgery for patients with Class III skeletal
Purpose: To evaluate subjective and objective outcomes of patients receiving Techmedica (currently TMJ Concepts) patient-fitted temporomandibular joint (TMJ) total joint replacement (TJR) devices after 19
The purpose of this study was to evaluate patients requiring unilateral total temporomandibular joint (TMJ).

5 Signs You May be Suffering from Obstructive Sleep Apnea Sleep apnea is one of the most prevalent sleep disorders in existence. However, it is

Everyone experiences jaw pain from time to time, but the cause and subsequent treatment range from ibuprofen to surgery. But how do you know if

Computational fluid dynamics for the assessment of upper airway changes in skeletal Class III patients treated with mandibular setback surgery.

Chapter 133 – Combined TMJ and Orthognathic Surgery
Protocol for Concomitant Temporomandibular Joint Custom – fitted Total Joint Reconstruction and Orthognathic Surgery Using Computer-assisted Surgical Simulation
Low Condylectomy and Orthognathic Surgery to Treat Mandibular Condylar Osteochondroma: A Retrospective Review of 37 Cases
A Classification System for Conditions Causing Condylar Hyperplasia

Protocol for Concomitant Temporomandibular Joint Custom-Fitted Total Joint Reconstruction and Orthognathic Surgery Utilizing Computer-Assisted Surgical Simulation
Outcome Assessment of 603 Cases of Concomitant Inferior Turbinectomy and Le Fort I Osteotomy
