Common Symptoms
- Anterior open bite
- Inability to bite into food
- Chronic jaw pain
- Severe restriction in jaw opening and movement
- Headaches
- Complete lip incompetence (inability to close lips at rest)
- Habitual mouth breathing
- Sleep disruption and inability to breathe through the nose during sleep
- Constricted airway
- Difficulty chewing
- Facial pain across the jaw, temples, and neck
- Progressive facial changes and chin recession
Procedure Performed
Bilateral Total Joint Replacement with Condylectomy. TMJ Fat Grafts. LeFort I Osteotomy. Genioglossus Advancement. Partial Bilateral Nasal Turbinectomies.
When the TMJs have deteriorated to end-stage disease, the damaged joints are removed and replaced with custom prosthetic joints. This is called Total Joint Replacement. The condylectomy is the removal of the damaged condyles. The prosthetic joints restore structure, function, and stability to the jaw.
TMJ Fat Grafts were harvested from the abdomen and placed around the new joints. The fat acts as a cushion and helps prevent scar tissue from forming around the prosthetic components.
A LeFort I Osteotomy repositions the upper jaw. The maxilla is separated from the skull and moved into its correct position. This corrects the bite relationship between the upper and lower jaws and helps open the airway.
Genioglossus Advancement addresses the airway directly. The genioglossus is the main muscle of the tongue. It attaches to the inside of the chin. During this procedure, the attachment point is pulled forward, which pulls the tongue base forward and prevents it from falling back into the airway during sleep.
Partial Bilateral Nasal Turbinectomies reduced the size of the turbinates inside the nose to improve nasal airflow. When a patient is transitioning from habitual mouth breathing to nasal breathing, clear nasal passages are essential.
Condition
Bilateral TMJ Osteoarthritis with Condylar Resorption. Maxillary and Mandibular Retrognathia. Obstructive Sleep Apnea.
Idiopathic Condylar Resorption. Severe Maxillary and Mandibular Retrognathia. Anterior Open Bite.
The temporomandibular joints, or TMJs, are the two joints that connect the lower jaw to the skull. They allow you to open and close your mouth, chew, and speak. When these joints break down, the condyles, the rounded ends of the lower jaw bone, deteriorate and lose height. As the condyles shrink, the lower jaw moves backward and downward. The bite shifts. The airway narrows.
The word idiopathic means there is no identifiable cause. The joints simply begin breaking down on their own. It is more common in young women and it is progressive. Without treatment, the joints continue to deteriorate, the bite continues to change, and the airway continues to constrict. The jaw does not rebuild on its own. Once the joints reach end-stage disease, the only path to restored function is total joint replacement.
When both the upper and lower jaws are positioned too far back, this is called maxillary and mandibular retrognathia. The result is a receding chin, a constricted airway, and a bite that does not function properly.
In Whitney’s case, the retrognathia was severe. Her mandibular deficiency measured 19 to 20mm. Her upper jaw was also deficient. The combined effect was a skeletal framework that could not support normal bite function or healthy airway volume.
An anterior open bite occurs when the upper and lower front teeth do not make contact when the mouth is closed. In Whitney’s case, the open bite measured 11mm. She could not bite into food. The back teeth were carrying the full load of every chewing movement, which placed additional stress on joints that were already failing.
When the jaw falls back, the tongue and soft tissues follow, reducing the space available for air. Whitney’s airway measured 83 mm² at its narrowest point.
The average is 140 mm² or above.
Because her jaw had collapsed backward so far, Whitney could not close her lips or breathe through her nose. Her body had adapted to mouth breathing as its only option, including during sleep.
About This Patient
Whitney was 31 when she came to us with a severe anterior open bite. Her front teeth didn’t touch, making it impossible to bite into food. Her jaw joints had fully degenerated, and as they failed, her jaw collapsed backward and downward, pulling her bite apart and compressing her airway.
She couldn’t close her lips or breathe through her nose. Mouth breathing had become her only option, even during sleep. Eating was limited, jaw movement was restricted, and chronic pain across her face and neck had become part of daily life. It had progressed slowly enough that she had adapted to it.
Her airway was significantly constricted, roughly one-third of normal. Her quality of life was steadily declining, specifically in how she ate, breathed and slept. Her pain levels were increasing and pain episodes were becoming more frequent.
Dr. Movahed replaced both failed joints with total joint prosthetics, repositioned the upper jaw, advanced the tongue base to open the airway, and cleared the nasal passages to restore breathing.
Six months after surgery, her pain was gone. With her airway open and nasal breathing restored, her sleep finally had the conditions it needed to recover. By eighteen months, she shared that she weighed more than she had in seven years, her body finally able to absorb the nutrition it had been missing and begin to rebuild.

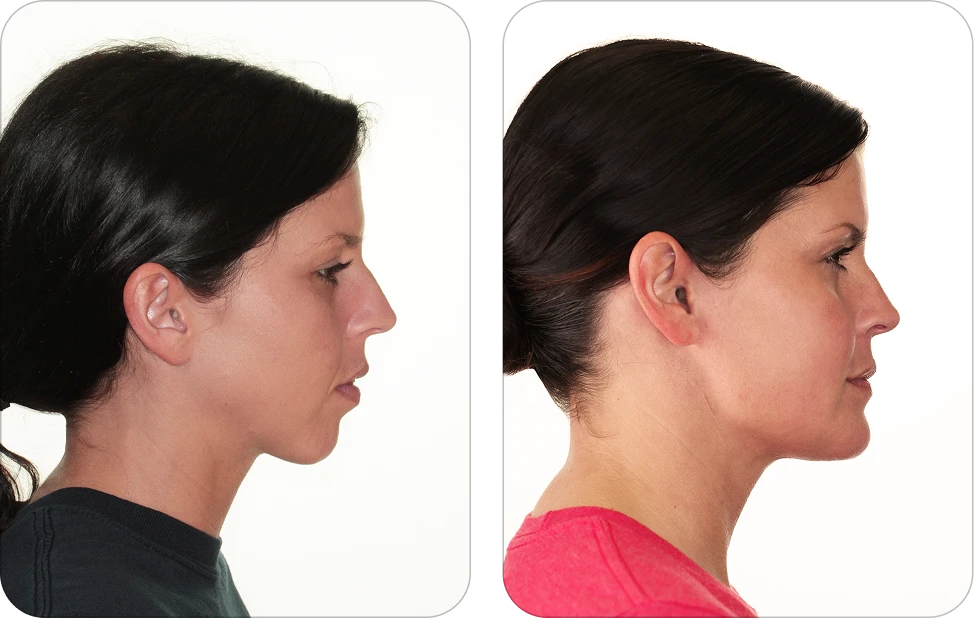
Before
After

